Rectal Bleeding (Blood in Stool)
What Is Rectal Bleeding?
Rectal bleeding, or blood in stool, is when blood is passed from the anus in your stool or on toilet paper. This is not normal and may be a sign of a conditions such as colorectal cancer, piles, or polyps.
Bright red blood usually indicates bleeding from the lower part of the digestive tract, while dark, tarry stools often suggests bleeding from the upper part of the tract.
Causes of Rectal Bleeding
There are several possible causes of rectal bleeding, ranging from anal fissures to colonic polyps and colorectal cancer.
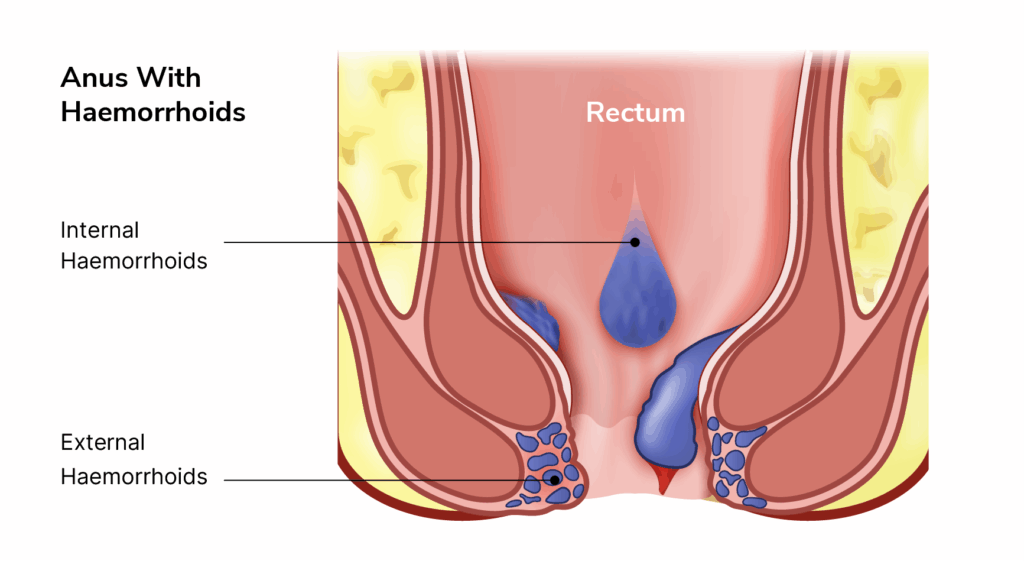
Haemorrhoids (Piles)
Haemorrhoids are swollen blood vessels around the anus that can bleed, itch, or feel like lumps. Straining during bowel movements or pregnancy often leads to haemorrhoids.
Learn more about haemorrhoids.
Anal Fissures
Anal fissures are small tears in the lining of the anus caused by passing hard stools. They typically cause sharp pain and bright red bleeding on the tissue or stool.
Diverticular Disease
Diverticula (small pockets) can form in the wall of the colon and may become inflamed or bleed. Diverticular bleeding is often painless but can be heavy.
Learn more about diverticular disease (diverticulitis).
Colitis and IBD
The colon can become inflamed from infections, ischemia, ulcerative colitis, IBD (inflammatory bowel disease), or Crohn’s disease. The inflammation can then cause bloody diarrhoea or bleeding.
Learn more about inflammatory bowel disease (IBS).
Angiodysplasia
Abnormal, fragile blood vessels in the colon can sometimes develop and cause painless bleeding. This is more common in older adults.
Colonic Polyps and Cancer
Benign growths (polyps) may develop in the colon and can sometimes bleed. If left untreated, some polyps may become cancerous and lead to changes in bowel habits.
Learn more about colon cancer.
How to Tell If You Have Rectal Bleeding (Blood in Stool)
Rectal bleeding or blood in the stool can often be noticed on toilet paper or in the stool after bowel movements. Below are the signs and symptoms to look for:
- Fresh, bright red blood coating the stool or toilet paper
- Dark red or black (“tarry”) stool
- Blood clots in stool
Depending on the cause of your rectal bleeding, it may be accompanied with the following symptoms:
- Itching, irritation or a tender lump at the anus
- Intense, tearing pain during bowel movements
- Changes in bowel habits, such as sudden, frequent diarrhoea or constipation
- Sudden presence of mucus in the stool
- A persistent sensation of incomplete bowel emptying
- Unintentional weight loss, fatigue or weakness
- Abdominal cramps or pain
See a Specialist about Rectal Bleeding
If you think you have rectal bleeding or are pooping blood clots, book an appointment with our colorectal specialist for proper medical examination, diagnosis, and treatment.
What to Be Concerned About with Rectal Bleeding
You should seek a doctor’s assessment for rectal bleeding if you observe any of the following, especially if you are over 50 or have a personal or family history of colorectal cancer or IBD:
- Heavy bleeding (eg. more than a teaspoon at a time)
- Prolonged bleeding (more than a day or two)
- Persistent or recurrent bleeding, which could indicate polyps or colorectal cancer
- Dark, black, or tarry stools, which may be a sign of upper gastrointestinal bleeding and need urgent evaluation
- Additional symptoms to go with your rectal bleeding, such as:
- Unexplained weight loss
- Significant fatigue (possible anaemia)
- Fever
- Severe abdominal pain along with bleeding are warning signs/li>
- Dizziness or weakness
How Rectal Bleeding Is Diagnosed
During the consultation, your doctor may request a detailed medical history and discuss your symptoms, including:
- The appearance, colour, and volume of the bleeding
- How often the bleeding occurs
- How long it has been present and whether it has changed over time
- Any potential triggers
- Whether other symptoms are present
During physical examination, your doctor will also examine the anus and lower rectum. This may involve the following:
- Visual inspection of the anal and rectal area
- A digital rectal examination to assess for masses or haemorrhoids
- Use of an anoscope or proctoscope to examine the anus and lower rectum
Depending on your condition, further tests may be recommended to identify the cause of rectal bleeding:
- Stool tests to detect hidden blood and assess for underlying conditions
- Blood tests to check for anaemia or infection
- An MRI or CT scan to locate the source of the bleeding
- An endoscopy (colonoscopy) for further inspection
Possible Treatments for Rectal Bleeding (Blood in Stool)
Treatment depends on the underlying cause and severity of the condition.
Self-care for Mild Rectal Bleeding and Discomfort
- Increase dietary fibre intake and maintain good hydration
- Use stool softeners to reduce straining and avoid irritation of the anal area
- Take warm sitz baths
- Maintain good anal hygiene
Medical Treatments for Persistent Rectal Bleeding or Pain
- Topical treatments to reduce inflammation and discomfort
- Pain relief medication, if appropriate
- Supplements such as iron, if the bleeding is leading to anaemia
Surgical Options for Serious Rectal Bleeding
Minimally invasive procedures such as rubber band ligation or sclerotherapy (injection) may be used to treat certain causes of rectal bleeding, particularly haemorrhoids.
In more serious or persistent cases, surgical intervention may be required to address the underlying condition and stop the bleeding. This is typically considered when rectal bleeding is linked to:
- Large or persistent haemorrhoids
- Polyps
- Tumours
- Diverticular bleeding
Discuss Your Treatment Options with a Specialist
Early detection and diagnosis can support timely and appropriate management of rectal bleeding. Book an appointment with our colorectal specialist for a thorough examination, diagnosis, and treatment plan for your condition.
